Is Diarrhea a Symptom of Pregnancy? Early Signs Explained
Pregnancy transforms your body in ways you might expect and many you don’t. While most people know about morning sickness and fatigue, fewer discuss what happens in your bathroom. Is diarrhea a symptom of pregnancy? The short answer is yes, but it’s not what you might think.
Throughout my career caring for patients navigating reproductive health concerns, I’ve observed that digestive changes—including both diarrhea and constipation—often accompany early pregnancy as progesterone and other hormones affect gastrointestinal motility. Many patients express confusion and concern when experiencing unexpected bowel changes, highlighting the importance of normalizing these conversations and providing clear guidance on distinguishing normal hormonal effects from symptoms requiring medical evaluation. I emphasize that while digestive symptoms can be part of the pregnancy picture, they should be assessed within the broader context of each individual’s health history and accompanying signs.
In this comprehensive guide, I’ll walk you through everything you need to know about pregnancy diarrhea early signs, when digestive problems during pregnancy are normal, and when they signal something requiring attention. Moreover, you’ll learn practical strategies to manage symptoms and protect both your health and your baby’s wellbeing.
Is Diarrhea a Symptom of Pregnancy? The Direct Answer
Let me be clear from the start. Yes, diarrhea can occur during pregnancy, but it’s not a primary or reliable pregnancy indicator. Furthermore, it’s actually less common than constipation in early pregnancy.
Is diarrhea a symptom of pregnancy that you should watch for? While hormonal fluctuations can cause loose stools, most women experience the opposite problem. Constipation affects 11 to 38 percent of pregnant women, particularly in the first and second trimesters. Nevertheless, some women do experience diarrhea, especially in these situations:
- Before a missed period, when hormones surge rapidly
- After starting prenatal vitamins
- When dietary habits change suddenly
- During times of high stress or anxiety
- In the final weeks before labor begins
If you’re wondering whether bowel changes as pregnancy symptom are normal, consider the complete picture. Diarrhea alone doesn’t confirm pregnancy. Instead, look for other signs like missed periods, breast tenderness, and fatigue.
💡 Pro Tip: Keep a symptom journal noting when digestive changes occur, what you ate, and other symptoms present. This helps identify patterns and provides valuable information for your healthcare provider.
Understanding Pregnancy Hormones and Bowel Movements
How Progesterone Affects Your Digestive System
Pregnancy hormones and bowel movements have an intricate relationship. Progesterone, the primary pregnancy hormone, typically slows your digestive system. Think of it as your body’s way of maximizing nutrient absorption for your growing baby.
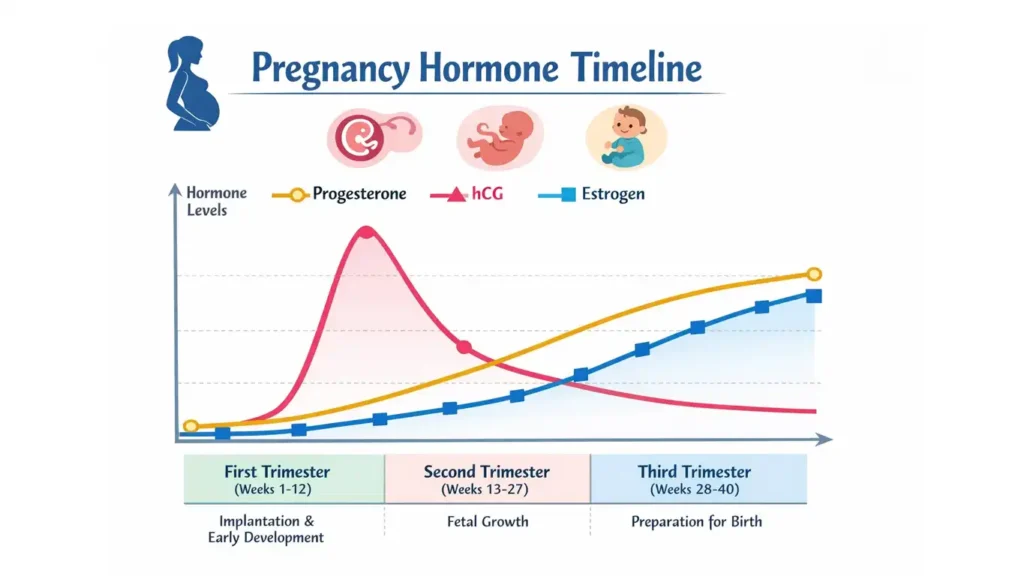
However, bodies respond differently. While most women experience slower digestion leading to constipation, some have the opposite reaction. Additionally, other hormones play a role:
- Human chorionic gonadotropin (hCG) rises rapidly in early pregnancy
- Estrogen increases significantly
- Prostaglandins can stimulate bowel activity
- Relaxin affects smooth muscle throughout your body
These pregnancy hormone effects on digestion create a unique experience for each woman. Consequently, your friend’s pregnancy digestive symptoms might look nothing like yours.
The Digestive System During Early Pregnancy
Your gastrointestinal tract undergoes remarkable changes even before you see that positive test. Blood volume increases by up to 50 percent during pregnancy. This affects every system, including your gut.

Early pregnancy stomach issues often include:
- Changes in appetite and food preferences
- Heightened sensitivity to smells
- Altered taste perception
- Variable bowel patterns
- Increased or decreased gastric motility
Can diarrhea be a sign of pregnancy before you’ve missed your period? Potentially, yes. Some women notice loose stools around implantation time, typically six to twelve days after conception. However, this symptom alone isn’t reliable enough to confirm pregnancy.
Diarrhea vs. Constipation: Understanding the Statistics
Most pregnancy resources focus heavily on constipation, and there’s good reason. Research shows constipation affects a significant portion of pregnant women, while diarrhea before missed period pregnancy scenarios are less commonly reported as primary symptoms.
Here’s what happens across trimesters:
First Trimester: Digestive symptoms vary wildly. Nausea affects approximately 90 percent of women. Meanwhile, some experience constipation while others have occasional loose stools. Hormonal surges create unpredictable responses.
Second Trimester: Constipation typically becomes more pronounced as progesterone levels remain elevated. Additionally, the growing uterus begins putting pressure on intestines. Diarrhea becomes less common during these middle months.
Third Trimester: Interestingly, loose stools may increase as your due date approaches. This happens because your body releases prostaglandins, preparing for labor. Therefore, pregnancy digestive changes by trimester follow recognizable patterns, though individual experiences vary.
Why do some women get diarrhea instead of constipation? Several factors influence this:
- Pre-existing digestive conditions like IBS
- Individual hormonal sensitivity
- Dietary changes upon learning about pregnancy
- Stress and anxiety levels
- Prenatal vitamin formulations
- Hydration status
Common Causes of First Trimester Diarrhea
Hormonal Fluctuations
Your body undergoes dramatic hormonal shifts in early pregnancy. These changes don’t just affect your reproductive system. Rather, they impact your entire body, including your gut.
The rapid rise in hormones can:
- Alter gut bacteria composition
- Change how quickly food moves through intestines
- Increase prostaglandin production
- Affect fluid balance in your colon
Some women notice digestive changes similar to what they experience before menstruation. If you typically get loose stools before your period, you might experience the same in early pregnancy.
Dietary Changes and Food Sensitivities
The moment you suspect pregnancy, eating habits often shift dramatically. Subsequently, your digestive system reacts to these changes.
Common dietary factors include:
- Suddenly increasing fiber intake
- Eating more fruits and vegetables
- Consuming different foods due to cravings or aversions
- Drinking more water
- Cutting out caffeine abruptly
- Developing temporary lactose sensitivity
Furthermore, food aversions can limit what you’re willing to eat. If you’re surviving on crackers and ginger ale, your bowel movements will change accordingly.
Prenatal Vitamins and Supplements
Starting prenatal vitamins represents a major dietary change. While iron in prenatal vitamins typically causes constipation, other components might have different effects.
Consider these factors:
- Magnesium content (a natural laxative)
- DHA and omega-3 supplements
- Folic acid in high doses
- Taking vitamins on an empty stomach
- Brand or formulation changes
If you suspect your prenatal vitamin is causing diarrhea and cramping early pregnancy, talk with your healthcare provider. Never stop taking prenatal vitamins without medical guidance, but you might benefit from a different formulation or timing.
💡 Pro Tip: Try taking your prenatal vitamin with your largest meal of the day or right before bed. This simple change can significantly reduce digestive side effects.
Stress and Anxiety
Your gut and brain communicate constantly through the gut-brain axis. Consequently, emotional states directly impact digestion.
Early pregnancy brings numerous stressors:
- Anxiety about pregnancy test results
- Worries about baby’s health
- Concerns about pregnancy complications
- Major life adjustments
- Financial considerations
This stress can manifest as is loose stool a sign of pregnancy that you’re experiencing? Sometimes, yes. However, it might also simply be stress-related digestive upset coinciding with early pregnancy.
When to Worry About Diarrhea in Pregnancy: Critical Red Flags
While occasional loose stools don’t typically signal problems, certain symptoms demand immediate medical attention. Therefore, understanding these red flags protects both you and your baby.
Signs of Infection or Illness
Call your healthcare provider immediately if diarrhea accompanies:
- Fever above 100.4°F (38°C)
- Severe, persistent abdominal cramping
- Blood or mucus in your stool
- Black, tarry stools
- Persistent vomiting preventing fluid intake
- Exposure to contaminated food or water
These symptoms suggest food poisoning, bacterial infection, or other conditions requiring prompt treatment. Certain infections pose serious risks during pregnancy, particularly Listeria, which can harm your developing baby.
Dehydration Warning Signs
Dehydration during pregnancy is particularly dangerous. Your body needs extra fluids to support increased blood volume and amniotic fluid. Moreover, severe dehydration can trigger preterm contractions.
Watch for these dehydration signs:
- Dark yellow or amber-colored urine
- Urinating less frequently than usual
- Dizziness when standing
- Dry mouth and cracked lips
- Rapid heartbeat or heart palpitations
- Extreme fatigue beyond normal pregnancy tiredness
- Decreased fetal movement (in later pregnancy)
If you notice these symptoms, contact your provider right away. You might need intravenous fluids to rehydrate safely.
Duration and Frequency Concerns
How long is too long? Generally, diarrhea lasting more than 24 to 48 hours warrants medical evaluation. Additionally, very frequent episodes—more than three in 24 hours—should prompt a call to your provider.
Are you experiencing progressively worsening symptoms? This pattern suggests something beyond simple hormonal adjustment. Furthermore, if you cannot keep fluids down due to combined vomiting and diarrhea, seek immediate care.
Conditions to Rule Out
When evaluating pregnancy gastrointestinal symptoms, healthcare providers consider several conditions:
- Food poisoning from contaminated food
- Viral gastroenteritis (stomach flu)
- Bacterial infections including Salmonella and E. coli
- Parasitic infections from contaminated water
- Inflammatory bowel disease flares
- Celiac disease reactions
- Urinary tract infections (surprisingly can cause digestive symptoms)
Each condition requires specific evaluation and treatment. Therefore, don’t try to self-diagnose or self-treat persistent symptoms.
Distinguishing Pregnancy-Related Diarrhea from Illness
How do you know if digestive problems during pregnancy stem from normal hormonal changes or actual illness? Ask yourself these questions:
- Did anyone else who ate the same food become ill?
- Have you traveled recently or consumed untreated water?
- Do you have fever, chills, or body aches?
- Is the diarrhea accompanied by severe, worsening pain?
- Are you seeing blood, mucus, or unusual colors in your stool?
- How long has this been happening?
Normal pregnancy-related loose stools typically:
- Occur occasionally, not constantly
- Resolve within a day or two
- Respond to dietary adjustments
- Don’t include fever or severe pain
- Maintain normal stool color
- Allow you to stay hydrated
Conversely, illness-related diarrhea usually:
- Comes on suddenly and severely
- Includes systemic symptoms like fever
- Contains blood or unusual colors
- Causes severe cramping
- Prevents adequate hydration
- Progressively worsens
When in doubt, call your healthcare provider. They’d rather answer questions and provide reassurance than have you delay necessary care.
The Diarrhea and Miscarriage Question
Many women worry: does diarrhea indicate miscarriage risk? Let me provide reassurance and clarity.
Diarrhea alone does not cause miscarriage. However, severe dehydration from persistent diarrhea can create complications. Additionally, certain infections that cause diarrhea might pose risks, which is why prompt medical evaluation matters.
Understanding the difference between cramping from diarrhea versus cramping from miscarriage helps reduce anxiety:
Diarrhea cramping:
- Comes in waves with bowel movements
- Improves after passing stool
- Located in lower abdomen
- Not accompanied by vaginal bleeding
Miscarriage warning signs:
- Heavy vaginal bleeding with clots
- Severe, persistent cramping
- Tissue passing from vagina
- Sudden loss of pregnancy symptoms
- Lower back pain combined with bleeding
Diarrhea is not a typical miscarriage symptom. Most miscarriages occur due to chromosomal abnormalities unrelated to digestive symptoms. Nevertheless, if you experience both diarrhea and any miscarriage warning signs, seek immediate medical evaluation.
Safe Management Strategies for Pregnancy Diarrhea
Immediate Home Care Steps

When facing loose stools during pregnancy, prioritize hydration above everything else. Your body and baby need adequate fluids.
Follow these steps:
- Drink clear liquids like water, clear broth, and herbal tea
- Try oral rehydration solutions designed to replace electrolytes
- Take small, frequent sips rather than large amounts at once
- Start the BRAT diet: Bananas, Rice, Applesauce, Toast
- Avoid dairy temporarily, as temporary lactose intolerance can occur
- Rest and allow your body to recover
Many women find that coconut water provides natural electrolyte replacement. Additionally, weak ginger tea can soothe both digestive upset and pregnancy nausea.
Foods to Eat and Avoid
Eat these foods:
- Bananas (high in potassium)
- White rice or oatmeal
- Applesauce (pectin helps firm stool)
- Toast or plain crackers
- Boiled potatoes
- Plain chicken or turkey
- Cooked carrots
- Probiotic yogurt (if tolerated)
Avoid these temporarily:
- Fatty or fried foods
- Spicy dishes
- Artificial sweeteners
- Caffeine
- Raw vegetables
- High-fiber foods
- Dairy (if causing problems)
- Sugary drinks and juices
Focus on bland, easily digestible options until symptoms resolve. Then, gradually reintroduce normal foods one at a time.
💡 Pro Tip: Keep frozen bananas on hand. They’re easy to digest, help firm stool, and can be soothing when you’re feeling queasy.
Hydration Protocol
Aim for at least eight to ten glasses of fluid daily when experiencing diarrhea. However, quality matters as much as quantity.
Best hydration choices:
- Plain water with a pinch of salt
- Coconut water
- Clear broth
- Herbal teas (ginger, peppermint)
- Oral rehydration solutions
- Diluted apple juice
Signs you’re adequately hydrated:
- Light yellow urine
- Urinating every few hours
- Moist mouth and lips
- No dizziness when standing
- Good energy levels
Electrolyte replacement becomes crucial when losing fluids through diarrhea. Therefore, plain water alone might not be sufficient. Sports drinks can work in moderation, but watch sugar content as excessive sugar can worsen diarrhea.
Medications and Supplements: What’s Safe During Pregnancy?
Over-the-Counter Considerations
Never take any medication during pregnancy without consulting your healthcare provider first. This includes seemingly harmless over-the-counter remedies.
Some providers may approve short-term use of:
- Kaolin-pectin preparations
- Loperamide (Imodium) in limited situations
- Probiotics (generally considered safe)
However, timing, dosage, and individual circumstances matter significantly. What’s appropriate for one pregnant woman might not be right for another.
What to Definitely Avoid

Bismuth subsalicylate (Pepto-Bismol) should be avoided during pregnancy. The salicylate component poses potential risks to developing babies. Additionally, many herbal remedies lack safety data in pregnancy.
Avoid these without medical approval:
- Most herbal supplements
- Excessive fiber supplements
- Stimulant laxatives
- Any medication not specifically approved by your provider
The general principle: when pregnant, less is more regarding medications. Try dietary and lifestyle modifications first.
Probiotic Considerations
Probiotics represent one of the safer options for supporting digestive health during pregnancy. Research suggests they may help:
- Restore healthy gut bacteria balance
- Reduce diarrhea duration
- Support immune function
- Possibly reduce gestational diabetes risk
Choose high-quality probiotic supplements with multiple strains. Alternatively, consume probiotic-rich foods like:
- Yogurt with live cultures
- Kefir
- Sauerkraut (pasteurized)
- Kimchi (pasteurized)
Always select pasteurized versions of fermented foods during pregnancy to avoid potential foodborne illness.
Adjusting Prenatal Vitamins
If prenatal vitamins seem to trigger symptoms, try these strategies:
- Take vitamins with your largest meal
- Split the dose (half morning, half evening)
- Try a different brand or formulation
- Switch to gummy vitamins temporarily
- Take right before bedtime
Never discontinue prenatal vitamins without provider guidance. Folic acid and other nutrients play critical roles in fetal development. However, adjusting how and when you take them can make a significant difference in tolerability.
Special Considerations: Pre-existing Digestive Conditions
Irritable Bowel Syndrome (IBS) and Pregnancy
If you have IBS before pregnancy, you might wonder how pregnancy affects symptoms. The answer varies significantly among women.
Some women with IBS-D (diarrhea-predominant) find symptoms improve during pregnancy. Others experience worsening. Progesterone’s effects on gut motility can go either way.
Management strategies include:
- Continuing safe IBS medications approved by your provider
- Following low-FODMAP diet modifications
- Managing stress through safe relaxation techniques
- Staying well-hydrated
- Working with both your OB and gastroenterologist
Document your symptoms carefully. This helps your healthcare team distinguish IBS flares from new pregnancy-related issues.
Inflammatory Bowel Disease (IBD)
Crohn’s disease and ulcerative colitis require careful management during pregnancy. Active disease poses more risks than the medications used to control it. Therefore, maintaining remission is crucial.
If you have IBD:
- Continue medications as directed by your gastroenterologist
- Report any symptom changes immediately
- Distinguish disease flares from normal pregnancy symptoms
- Attend all monitoring appointments
- Optimize nutrition carefully
Most IBD medications are compatible with pregnancy. However, some require adjustment. Never change medications without coordinated care from your OB and gastroenterologist.
Celiac Disease and Food Intolerances
Strict gluten-free diet adherence becomes even more important during pregnancy. Additionally, some women develop temporary lactose intolerance even without previous issues.
Key strategies:
- Read all labels meticulously
- Watch for cross-contamination
- Consider eliminating dairy temporarily if problems arise
- Ensure adequate nutrient intake from safe sources
- Work with a dietitian familiar with pregnancy needs
Uncontrolled celiac disease during pregnancy can affect nutrient absorption, potentially impacting fetal development. Therefore, strictness with your diet truly matters.
Comparing Digestive Symptoms in Pregnancy
Understanding where diarrhea fits among pregnancy digestive symptoms provides helpful perspective:
| Symptom | Timing | Prevalence | Typical Cause | Concern Level |
|---|---|---|---|---|
| Nausea/Vomiting | Weeks 4-16 | 90% of women | Hormones (hCG) | Low unless severe (hyperemesis) |
| Constipation | Throughout, peaks 2nd-3rd trimester | 11-38% | Progesterone, iron supplements | Low, manageable with diet/lifestyle |
| Diarrhea | Variable, increases near labor | Less common in early pregnancy | Multiple factors | Moderate if persistent or severe |
| Heartburn | 2nd-3rd trimester mainly | 17-45% | Progesterone, uterine pressure | Low, uncomfortable but manageable |
| Gas/Bloating | Throughout pregnancy | Very common | Progesterone, dietary changes | Low |
This comparison shows that while pregnancy symptoms diarrhea or constipation can occur, constipation predominates in most women. Nevertheless, both deserve attention and proper management.
Practical Tips for Managing Digestive Health During Pregnancy
Daily Habits That Help
Consistency in daily routines supports digestive health throughout pregnancy. Therefore, establish these beneficial habits:
- Eat regular meals at consistent times
- Stay hydrated throughout the day, not just when thirsty
- Walk daily to support healthy gut motility
- Practice stress reduction through safe techniques like prenatal yoga
- Sleep adequately as fatigue worsens all symptoms
- Keep a food diary to identify trigger foods
Small changes accumulate into significant improvements. Furthermore, these habits benefit your overall pregnancy health beyond just digestive concerns.
Dietary Strategies
Nutrition during pregnancy affects everything from energy levels to digestive comfort. Consider these approaches:
- Eat smaller, more frequent meals rather than three large ones
- Balance proteins, fats, and carbohydrates at each meal
- Avoid known trigger foods that worsen symptoms
- Ensure food safety through proper storage and cooking
- Read labels carefully to avoid problematic ingredients
- Wash produce thoroughly to prevent foodborne illness
Additionally, gentle cooking methods like steaming or baking tend to be easier on sensitive digestive systems than frying or heavy seasoning.
Lifestyle Modifications
Beyond what you eat, how you eat matters:
- Eat slowly and chew thoroughly
- Don’t lie down immediately after meals
- Take a gentle walk after eating to aid digestion
- Practice mindful eating without distractions
- Manage stress through safe relaxation techniques
- Connect with support systems for emotional wellbeing
These simple modifications can significantly impact digestive comfort. Moreover, they promote overall wellness during pregnancy.
The Mind-Gut Connection in Pregnancy
How Stress Affects Digestion
The vagus nerve creates a direct communication highway between your brain and gut. Consequently, emotional states produce physical digestive responses.
Pregnancy brings unique stressors:
- Anxiety about baby’s health and development
- Financial concerns
- Relationship adjustments
- Career considerations
- Physical discomfort and changes
These worries can manifest as digestive symptoms, including loose stools. Furthermore, the stress-symptom cycle can perpetuate itself. Digestive problems cause anxiety, which worsens digestive problems.
Mental Health Support
Breaking this cycle requires addressing both physical and emotional aspects. Consider these approaches:
- Talk with your healthcare provider about pregnancy anxieties
- Join prenatal support groups to connect with others
- Practice relaxation techniques like deep breathing
- Try prenatal yoga designed for pregnant women
- Consider counseling if anxiety feels overwhelming
- Involve your partner in emotional processing
Mental health significantly impacts physical health, especially during pregnancy. Therefore, addressing anxiety and stress isn’t optional; it’s essential healthcare.
Preparing for Labor: Late Pregnancy Diarrhea
Is Diarrhea a Sign of Labor?
As your due date approaches, loose stools often increase. This represents your body’s natural preparation for birth. Specifically, prostaglandins released before labor stimulate bowel activity.
Many women experience diarrhea 24 to 48 hours before labor begins. This happens because:
- Prostaglandins soften the cervix and stimulate contractions
- These same hormones affect intestinal smooth muscle
- Your body naturally “clears out” before delivery
- Hormonal shifts change gut motility
Other pre-labor signs to watch for:
- Increased Braxton Hicks contractions
- Mucus plug loss (bloody show)
- Water breaking
- Regular contractions increasing in intensity
- Lower back pain
- Nesting instinct intensifying
If you’re full-term and experiencing loose stools combined with other labor signs, contact your provider. However, diarrhea alone doesn’t necessarily mean labor is imminent.
What Healthcare Providers Want You to Know
Communication is Key
Throughout my career, I’ve learned that the best patient outcomes occur when communication flows freely. Therefore, I encourage every pregnant woman to:
- Never hesitate to call with concerns
- Ask questions no matter how simple they seem
- Report all symptoms honestly and completely
- Follow up if symptoms change or worsen
- Know after-hours protocols before emergencies arise
Your healthcare provider would rather answer ten unnecessary questions than miss one important symptom. Furthermore, prenatal care works best as a partnership built on open dialogue.
Keeping Track of Symptoms
Maintaining a symptom journal provides valuable information for your healthcare team. Record these details:
- Frequency: How many episodes in 24 hours?
- Timing: When do symptoms occur relative to meals?
- Stool characteristics: Color, consistency, presence of blood or mucus
- Associated symptoms: Cramping, fever, nausea?
- Foods consumed: What did you eat in the previous 24 hours?
- Hydration status: Urine color and frequency
This documentation helps identify patterns you might not otherwise notice. Additionally, it provides concrete information when discussing symptoms with your provider.
Prevention Strategies for Digestive Comfort
Before Pregnancy (If Planning)
If you’re planning pregnancy, optimize digestive health beforehand:
- Take probiotics to establish healthy gut bacteria
- Identify food sensitivities through elimination diets
- Manage pre-existing conditions like IBS or IBD
- Build healthy eating habits before hormonal changes complicate things
- Stay well-hydrated as a baseline practice
Starting pregnancy with optimal digestive health provides a better foundation for managing inevitable changes.
Throughout Pregnancy
Consistency matters more than perfection. Focus on:
- Maintaining regular eating patterns even when appetite varies
- Making dietary changes gradually to allow digestive adaptation
- Attending all prenatal appointments for monitoring
- Communicating openly with your healthcare team
- Staying informed without becoming anxious
- Prioritizing self-care through rest and stress management
These strategies support both digestive health and overall pregnancy wellbeing.
Common Myths and Misconceptions
Myth: Diarrhea Means Something is Wrong with Baby
Truth: Maternal digestive issues rarely affect fetal health directly. Your baby is protected by the placenta and amniotic fluid. Furthermore, most pregnancy-related diarrhea stems from hormonal changes, dietary adjustments, or minor infections that don’t cross the placental barrier.

However, severe dehydration can reduce blood flow to the uterus. This is why staying hydrated matters so much. Additionally, certain serious infections require treatment to protect your baby. Therefore, while diarrhea itself doesn’t harm your baby, the underlying cause might need evaluation.
Myth: You Should Just Tough It Out
Truth: Suffering unnecessarily helps no one. Safe treatment options exist for managing digestive symptoms during pregnancy. Moreover, quality of life during pregnancy truly matters.
Dehydration poses real risks including:
- Preterm contractions
- Reduced amniotic fluid
- Decreased blood volume
- Electrolyte imbalances
- Kidney problems
Seeking appropriate medical care isn’t weakness. Rather, it’s responsible pregnancy management that protects both you and your baby.
Myth: All Digestive Issues Signal Hyperemesis or Serious Conditions
Truth: Most digestive symptoms during pregnancy are normal, manageable, and temporary. Hyperemesis gravidarum primarily involves severe, persistent vomiting, not diarrhea. While it’s a serious condition requiring treatment, it’s also relatively rare, affecting only 0.3 to 3 percent of pregnancies.
The vast majority of digestive changes during pregnancy are uncomfortable but not dangerous. Nevertheless, knowing the difference between normal and concerning symptoms empowers you to seek appropriate care when needed.
Conclusion: Navigating Digestive Changes with Confidence
So, is diarrhea a symptom of pregnancy? Yes, it can be, though it’s less common and less reliable than other early signs. While most women experience constipation due to rising progesterone levels, some do encounter loose stools, particularly during hormonal surges or near labor.
The key takeaways:
- Diarrhea can occur in early pregnancy but isn’t a primary indicator
- Hormonal changes affect everyone differently
- Hydration remains your top priority
- Most cases are benign and manageable at home
- Red flags require prompt medical evaluation
- Your healthcare team is there to support you
Throughout my years caring for patients, I’ve seen that knowledge reduces anxiety. Understanding what’s normal versus concerning empowers you to trust your body while also knowing when to seek help. Furthermore, remember that every pregnancy journey is unique. Your experience might differ from your friend’s, your sister’s, or even your own previous pregnancies.
Don’t hesitate to reach out to your healthcare provider with questions or concerns. We’d much rather provide reassurance and guidance than have you worry in silence. Your comfort, health, and peace of mind during pregnancy matter tremendously.
If you’re experiencing digestive changes that concern you, make that call. Trust your instincts. You know your body better than anyone else. Together with your healthcare team, you can navigate these changes confidently, ensuring the healthiest possible pregnancy for both you and your baby.

















