Estimated Reading Time: 9 Minutes
I have spent decades covering the wellness beat, and if there is one thing I have learned, it is that we are suffering in silence. We treat our backs, our hearts, and our skin, but we often ignore the very core of our anatomy until it screams for attention. Specifically, I am talking about Pelvic Floor Health. It is the missing link in the conversation about why we leak when we laugh, why intimacy might hurt, and why we wake up three times a night to use the bathroom.
Unfortunately, for too long, we have accepted these issues as a normal part of aging or motherhood. We have been told to “just live with it” or, conversely, to just do a few Kegels and hope for the best. However, that advice is outdated, and frankly, it is often wrong.
In this deep dive, we are going to unpack the complex relationship between your bladder, your muscles, and your sex life. We are drawing insights from the “Dream Team for Down There”—Dr. Rena Malik, a reconstructive urologist, and Dr. Sonia Bahlani, a pelvic pain specialist and gynecologist. Together, we will explore why you might be misdiagnosing your own symptoms and, essentially, how simple changes can revolutionize your quality of life.
The Bladder Breakdown: Pelvic Floor Health and Leaks
Let’s start with the bladder. It is the organ that dictates our schedule, our travel plans, and our confidence. When I speak to women (and men) about their daily lives, the fear of leakage is a constant, low-level anxiety. But to fix it, you have to understand what is actually breaking down.

Specifically, we generally see two types of Urinary Incontinence: First, there is stress incontinence. This is the physical failure of the closure mechanism. For example, you cough, you sneeze, you lift a heavy box, and subsequently, you leak. The pressure in your abdomen overwhelms the urethral sphincter. Second, there is urgency incontinence. This is the “gotta go, gotta go” sensation where your bladder contracts before you are ready.
So, why does this happen?
In reality, it is rarely just one thing. It is often a combination of weak muscles and lifestyle triggers.
Assessing Your Habits
For instance, consider your hydration habits. We live in a culture that worships the giant water bottle. We carry liters of water around like security blankets. However, Dr. Malik points out a critical error here: if you over-drink, you over-void.
💡 Pro Tip: Stop chugging. Sip your water throughout the day. If you overwhelm your system with massive gulps, your kidneys process it rapidly, and your bladder fills too quickly. Aim for steady hydration, not a flood. 📈
Furthermore, we need to talk about constipation. The pelvis is like a small apartment. If the rectum is full of stool, it pushes against the bladder. This is the “full house” effect. Consequently, you cannot achieve optimal Urinary Incontinence Treatment if you are chronically constipated. The pressure confuses the bladder nerves, leading to urgency and leaks.
Dietary Triggers to Watch
Have you considered that your morning routine might be the culprit? Dr. Malik highlights that coffee and Chai—staples in many of our diets—are significant Bladder Irritants. Caffeine acts as a diuretic, filling the bladder faster. Moreover, the acidity irritates the bladder lining, causing it to spasm. This creates a perfect storm for urgency.
When It’s Not a UTI: Pelvic Floor Health and Bladder Pain
One of the most frustrating narratives I encounter in medical journalism is the woman who has had ten UTIs in a year, yet her cultures always come back negative. She takes round after round of antibiotics, but the burning and urgency never truly leave.
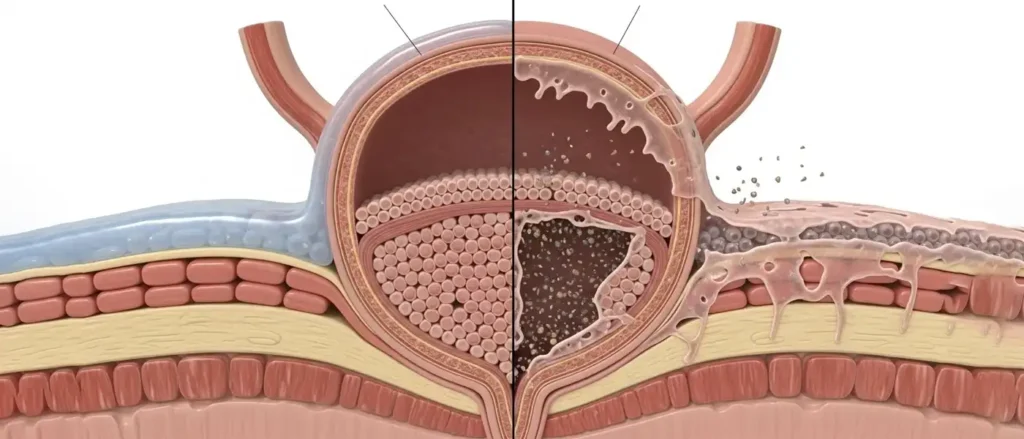
This is often a case of mistaken identity. It looks like an infection, but it is actually Interstitial Cystitis (IC), also known as Bladder Pain Syndrome.
The difference is crucial. A UTI is a bacterial infection. Conversely, IC is a chronic condition involving the bladder wall itself. Dr. Bahlani uses a brilliant analogy: think of your bladder lining like a waterproof coat. In a healthy bladder, this coat (the GAG layer) protects the nerves from the acid in your urine. However, in patients with IC, this coat has holes in it. It is like “leaky gut” for the bladder.
When you eat spicy food or drink alcohol, those irritants seep through the defective lining and hit the raw nerves underneath. As a result, you feel pain as the bladder fills.
This distinction matters because the treatment for Interstitial Cystitis vs UTI is completely different. Antibiotics do nothing for IC and can actually harm your gut microbiome. Instead, management involves identifying food triggers and calming the nervous system. Therefore, if you have pain while your bladder is filling, rather than just burning when you pee, you need to ask your doctor about IC.
The Pelvic Floor Health Connection: The “TMJ” of the Pelvis
Now, let’s get to the muscles. This is where the concept of High Tone Pelvic Floor dysfunction comes into play.
Most people assume that if they have bladder issues, their muscles must be “loose” or weak. Therefore, they think they need to tighten up. But Dr. Bahlani compares the pelvic floor to the jaw. When you are stressed, do you clench your teeth? Many of us do the exact same thing with our pelvis. We hold tension in those muscles without realizing it.
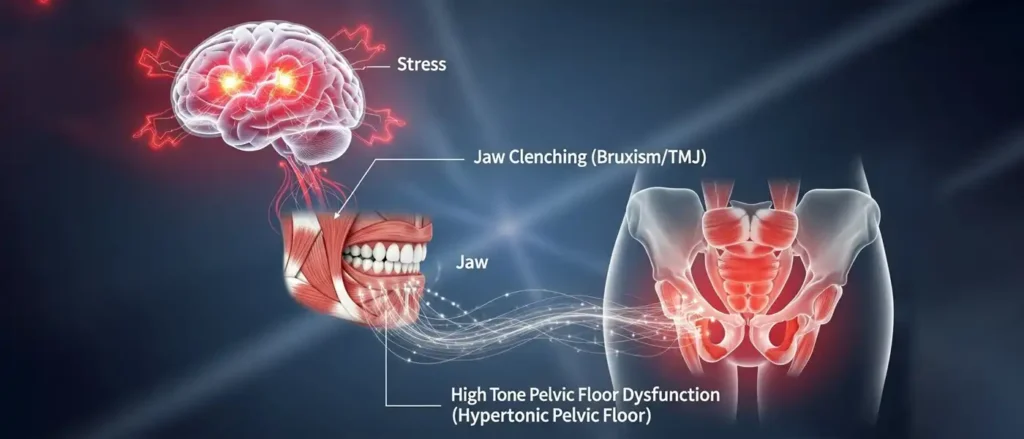
This leads to a hypertonic, or “high tone,” pelvic floor. These muscles are short, tight, and exhausted. They are not weak; they are overworked.
Here is the paradox: a tight muscle is a weak muscle. If your pelvic floor is clenched tight 24/7, it cannot react when you sneeze. It is already maxed out. Consequently, you leak. This is where Dysfunction sets in.
The Kegel Misconception
This brings us to the biggest myth in pelvic health: the Kegel.
💡 Pro Tip: If you have pelvic pain or urgency, stop doing Kegels immediately. Strengthening a tight muscle is like trying to do a bicep curl with a cramped arm. You need to learn to relax (Reverse Kegels) before you can strengthen. 🗣️
For many patients, Pelvic Floor Health isn’t about gym-style workouts. Rather, it is about down-training the nervous system. It is about teaching those muscles to let go. This is why physical therapy is essential. A specialized therapist can identify if you are “short and tight” or “long and weak.” Guessing at home often makes the problem worse.
Advanced Medical Interventions for Pelvic Floor Health
Sometimes, lifestyle changes and physical therapy aren’t enough. Fortunately, medical science has advanced significantly. We no longer have to rely solely on major surgeries with long recovery times.
For bladder control, Botox is a game-changer. Just as Botox relaxes wrinkles in the forehead, similarly, it can relax the bladder muscle. This prevents the spasms that cause urgency and leakage. It is a quick office procedure that can provide relief for months.
Another fascinating option is Sacral Neuromodulation, essentially a “pacemaker” for the bladder. It corrects the electrical signals between the bladder and the brain. If the wiring is faulty, the device helps normalize the signal.
Additionally, Dr. Malik mentions PTNS (Percutaneous Tibial Nerve Stimulation). This is like acupuncture for your bladder. A tiny needle in the ankle stimulates a nerve that travels up the leg to the sacrum, calming the bladder. It is non-invasive and highly effective for overactive bladder symptoms. These options prove that you don’t have to live in diapers or fear leaving your house.
Reclaiming Intimacy: Pelvic Floor Health and Sex
Finally, we must address the elephant in the room: sex.
Painful intercourse, or Dyspareunia, is a massive quality-of-life issue that is rarely discussed. In many cultures, especially the South Asian communities Dr. Malik and Dr. Bahlani serve, female pleasure and pain are treated as taboo. But historically, texts like the Kamasutra celebrated sexual wellness. Therefore, we need to reclaim that openness.

Pain during sex can stem from multiple sources. It could be Vulvodynia, a chronic pain condition at the vaginal opening. Alternatively, it could be hormonal changes thinning the tissue. Or, very often, it is that same high-tone pelvic floor. If the muscles are clenched shut, penetration is going to hurt. This can spiral into Vaginismus, where the muscles spasm involuntarily to protect you from pain.
Female Sexual Wellness relies on blood flow and relaxation. This is where lubrication becomes a medical necessity, not just a “fun” add-on.
Tools for Pleasure
Dr. Bahlani advises avoiding lubricants with parabens and glycerin, which can irritate sensitive tissue. Silicone-based lubes are excellent because they don’t dry out and offer a silky barrier. In a pinch, natural oils like coconut oil or even vegetable shortening (like Crisco) can be incredibly soothing for women with significant dryness or atrophy.
Furthermore, we need to talk about vibrators. Dr. Malik prescribes them. Yes, you read that right. A small vibrator is not just a toy; it is a therapeutic device. The vibration increases blood flow to the pelvic region, which promotes healing and tissue health. Additionally, it helps with desensitization if you have pain.
💡 Pro Tip: 80% of women require clitoral stimulation to reach orgasm. This is simple anatomy, not a dysfunction. Using tools like vibrators to bridge the “orgasm gap” is a healthy, normal part of sexual function. 🗣️
Can we stop pretending that suffering through sex is a duty?
If sex hurts, your body is telling you something is wrong. Whether it is Vaginismus Treatment through dilation therapy, hormonal creams, or pelvic floor relaxation techniques, there is a path back to pleasure.
Conclusion
Ultimately, Pelvic Floor Health is not a luxury; it is the foundation of your daily comfort and your most intimate moments. The connection between a stressed mind, a clenched pelvis, and a reactive bladder is undeniable.

First, we explored how Bladder Irritants like coffee can sabotage your day. Next, we looked at the difference between Interstitial Cystitis and infections. Finally, we debunked the idea that Kegels are a cure-all for Hypertonic Pelvic Floor issues.
The most important takeaway is this: you are your own best advocate. If you are leaking urine, it is not normal. Similarly, if sex is painful, it is not normal. These are treatable medical conditions.
Dr. Rena Malik and Dr. Sonia Bahlani represent a new wave of medicine that looks at the whole person—the diet, the stress levels, the muscles, and the nerves. You don’t have to accept a life of “just getting by.”
Therefore, prioritize your self-care. Whether that means taking ten minutes for meditation to lower your cortisol, swapping your second coffee for water, or booking an appointment with a urologist, take that step today. You deserve to live pain-free.
















