I often see patients who feel they are doing everything right. You might be eating the same way and moving the same way as you did ten years ago, yet you find yourself gaining weight out of nowhere. This “doing everything right” paradox is a common frustration for those navigating the silent shift in midlife health. As a seasoned urologist and Clinical Professor at NYU Grossman School of Medicine, I believe it is vital to understand that your sexual and urologic health are deeply connected to your metabolic state. Sexual Dysfunction in Midlife is not just an isolated issue; it is often a window into your overall wellbeing.
My approach at NYU Langone is patient-centered, focusing on improving your quality of life by relieving pain, resolving infections, and addressing both sexual and urinary dysfunction. Through decades of experience and leadership in the American Urological Association, I have learned that a holistic view is necessary. We must bridge the gap between weight management and genitourinary health to provide the best care.

Pro Tip: Keep a daily log of your energy levels and any changes in urinary habits to help us identify patterns early. 📝
Understanding Obesity as a Metabolic Disease
When we talk about weight, we must look beyond the scale. I encourage you to shift your perspective from viewing weight as a “willpower” issue to seeing it as part of a metabolic disease spectrum. This is especially important as we age because obesity involves many factors beyond just calories in and calories out.
Hormones play a critical role in how your body manages energy. Insulin, for example, is a key signaling agent that tells your body how to store and use fuel. Furthermore, fat tissue is not just stored energy; it is hormonally active. It can drive insulin resistance and even affect your “fullness” hormones, like leptin, making you feel hungry even when you have eaten enough.
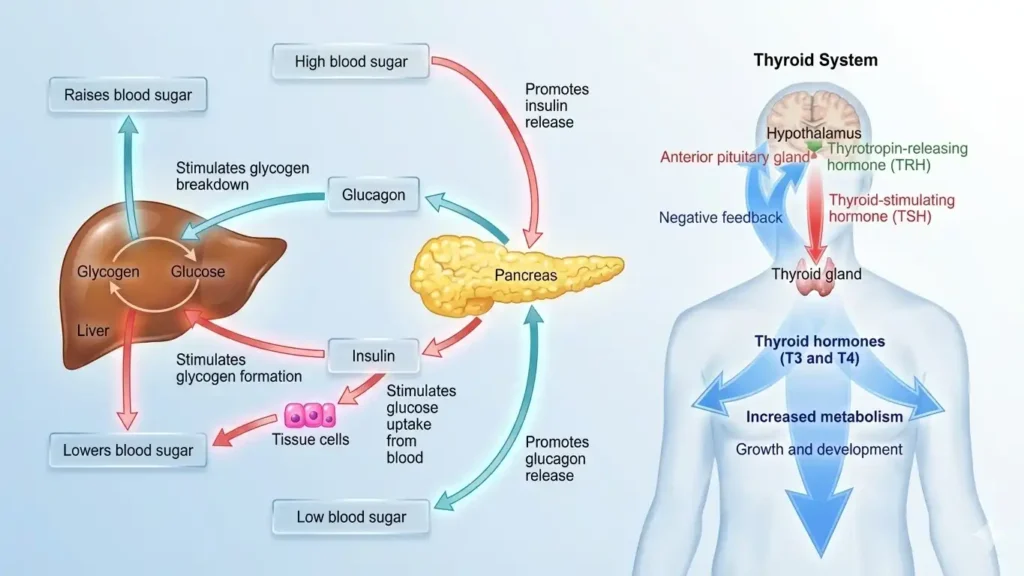
Why does understanding these hormonal triggers help you feel more in control of your health?
The Menopause Transition: Why the Body Composition Changes
For many women, the transition to menopause brings a noticeable change in where the body stores fat. As estrogen levels decline, you may see an increase in insulin resistance, which leads to weight gain specifically in the abdomen. This “softness” in the middle, often called visceral fat, is actually weight gain happening in and around your organs.
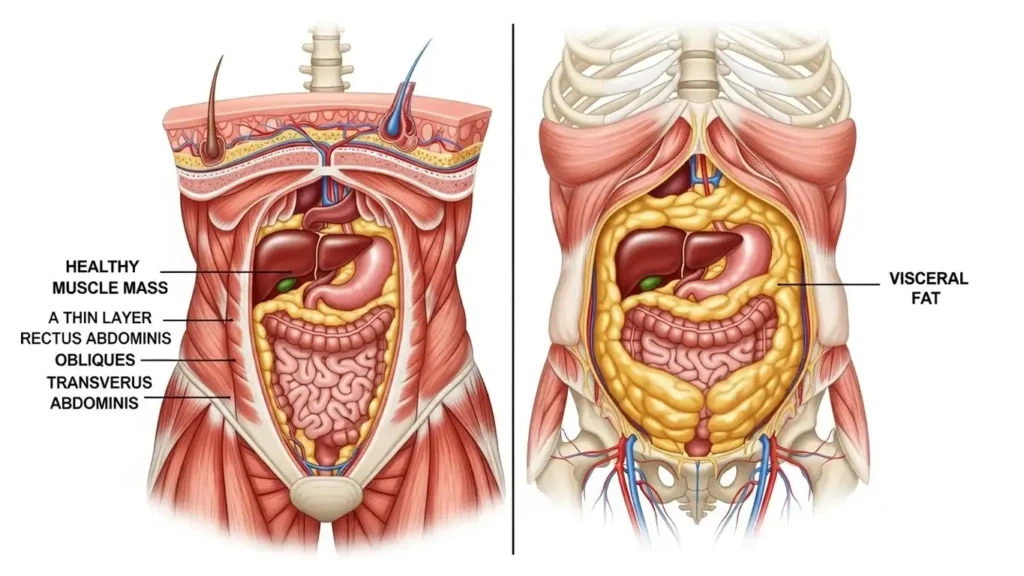
The Role of Muscle and Vascular Health
- As we get older, there is a natural decline in muscle mass.
- Muscle burns more energy than fat, so losing muscle slows down your metabolic rate.
- Visceral fat increases the risk of heart disease and vascular issues.
- Maintaining metabolic health is crucial to prevent the progression of Sexual Dysfunction in Midlife.
The Impact of Weight on Sexual and Urologic Health
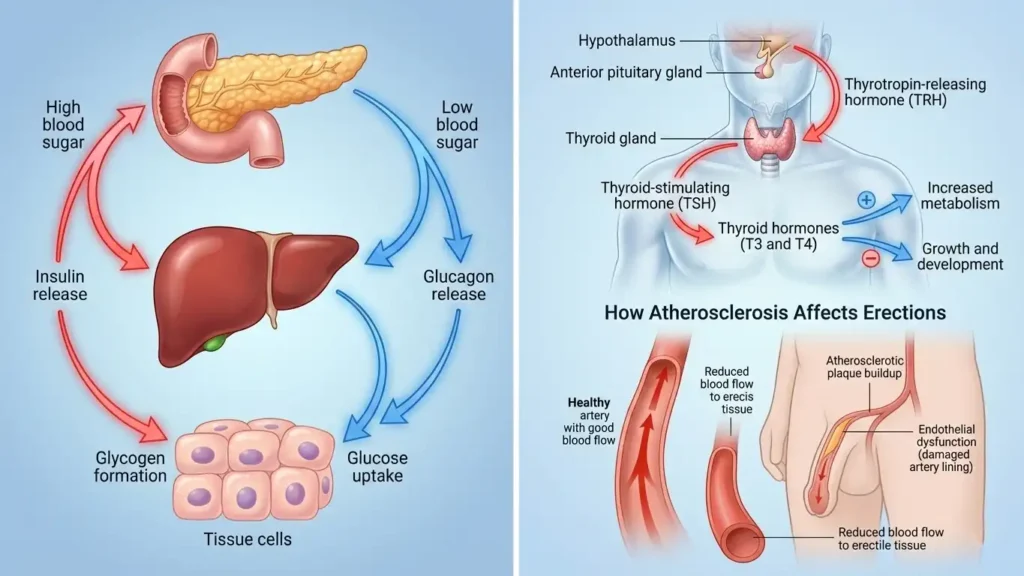
Obesity affects your sexual health through both hormonal and physiological pathways. Increased fat mass can change your active sex hormone levels, leading to an imbalance in estrogen and testosterone. For many, Sexual Dysfunction in Midlife can be a warning sign of deeper cardiovascular or metabolic issues.
For instance, erectile dysfunction is often one of the first signs of cardiac disease. If the small vessels that support an erection are struggling, it may mean the arteries to your heart need attention too. Psychological factors also matter; how you feel about your body directly impacts your comfort and safety during intimacy.
Pro Tip: Prioritize open communication with your partner about physical changes to reduce the emotional burden of midlife transitions. 🗣️
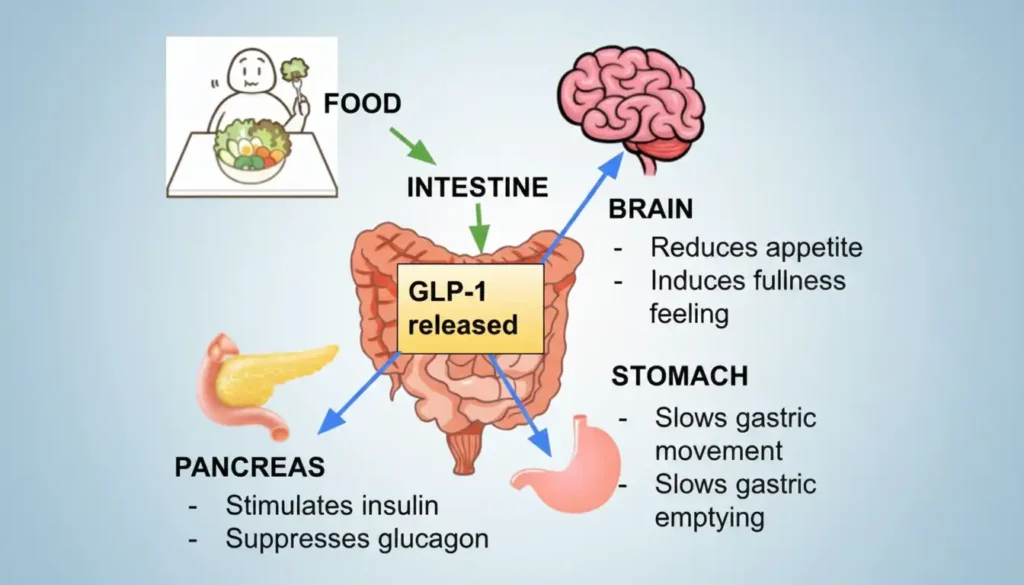
GLP-1 Medications: A New Frontier in Treatment
New tools like GLP-1 receptor agonists, such as semaglutide and tirzepatide, are changing how we treat obesity. These medications work by slowing down how fast your stomach empties and acting on brain receptors to reduce “food noise” or constant cravings.
Beyond weight loss, these medications offer significant cardiovascular benefits. In many cases, they can be used alongside Hormone Replacement Therapy (HRT) to improve metabolic outcomes. By stabilizing your metabolic health, we can often see improvements in Sexual Dysfunction in Midlife.
How could a combined approach to hormones and weight loss change your daily energy?
Addressing Treatment Nuances and Patient Concerns
While GLP-1s are powerful, we must watch for side effects like “apathy” or a loss of pleasure, sometimes called anhedonia. Because these medications work in the brain, they can sometimes affect your mood or desire. It is also vital to manage rapid weight loss risks by protecting your muscle mass through proper protein intake and exercise.
One common myth is that you should always use the smallest dose possible, often called “microdosing”. In reality, finding the right dose for your body is what matters most to avoid feeling “overtreated” or exhausted.
Pro Tip: Ensure you are getting enough fiber and healthy fats to support your brain health and hormone production during weight loss. 🥑
Clinical Leadership and Policy: The Importance of Expert Care
Seeking care from a board-certified specialist is essential for your safety. My role as a Clinical Professor and my involvement with the AUA board of directors allow me to stay at the forefront of urologic policy and care delivery. We aim to provide durable outcomes using innovative, minimally invasive techniques for conditions like Sexual Dysfunction in Midlife, kidney stones, and Benign Prostatic Hyperplasia (BPH).
Why is it important to have a specialist who understands the link between your metabolism and your urologic health?

Reclaiming Your Quality of Life
You do not have to settle for pain or dysfunction. Modern endourologic and minimally invasive treatments can resolve infections, manage an enlarged prostate, and restore your vitality. By addressing the metabolic hurdles together, we can improve your overall Urologic Wellness. I encourage you to speak up and consult with a professional to start your journey back to health.















