In my years as a reconstructive urologist, I have seen how much stress a single medical report can cause. Today, many of my patients ask about the latest trends in “preventative” scanning. You might have seen celebrities or influencers posting about getting a full-body scan to “catch everything early.” It sounds like a great idea, doesn’t it? However, as we look closer at prostate MRI screening benefits, we start to see that “more” is not always “better.” This post will help you understand why targeted, evidence-based imaging is safer for your health and your peace of mind than a random, expensive search for problems that may not exist.
The Allure of the “Perfect” Scan
The Celebrity Trend vs. Medical Reality Lately, social media is full of people claiming that a $2,500 full-body MRI saved their lives. They promise that scanning every inch of your body provides ultimate peace of mind. It is a seductive core promise: the belief that looking everywhere will catch a “silent killer” before it strikes. But is this reality, or just a high-priced marketing campaign?
The Expert Verdict I often discuss this with colleagues like Dr. Matthew Davenport and Dr. Rena Malik. We look at the data, not the hype. Medical societies do not endorse full-body MRIs for people who feel healthy. Why? Because these scans often cause more harm than good through overdiagnosis and unnecessary procedures. While the technology is amazing, using it without a specific reason is like using a magnifying glass to find dust in a clean room—eventually, you will find something, even if it doesn’t matter.
Pro Tip: Before booking any elective scan, ask your doctor if the results will actually change your treatment plan. 📋
What Actually Is a Full Body MRI?
Understanding the Technology To understand prostate MRI screening benefits, we must first understand what an MRI is. Magnetic Resonance Imaging uses very strong magnets to take detailed pictures of your soft tissues. This includes your brain, liver, and muscles.
MRI vs. CT vs. PET
- MRI: This uses no ionizing radiation. It is the gold standard for looking at soft tissues.
- CT Scan: This uses X-rays (radiation). It is great for looking at bones or for quick emergency checks.
- PET Scan: This looks at how your body uses sugar. It helps find active cancer cells but involves radiation.
The Commercial Scan Limitations Most “boutique” scan companies do their work without contrast dye. They do this to avoid the need for IVs and extra medical staff. However, without contrast, a radiologist often cannot tell the difference between a harmless fluid-filled cyst and a solid tumor. This leads to immediate uncertainty. Have you ever wondered why these companies don’t usually accept insurance? It is because insurance only pays for tests that are medically necessary.
The Hidden Dangers of Screening the “Healthy”
The Problem of “Incidentalomas” When we scan healthy people, we find “incidentalomas.” These are spots or lumps found by accident. Statistics show that 20% to 40% of abdominal scans in healthy people find something. These “incidental findings” are usually harmless, but they look suspicious enough that we feel forced to test them.
Pre-Test Probability If you have no symptoms, the “pre-test probability” of having a deadly disease is low. This means that if the scan finds a spot, it is much more likely to be a false alarm than a real emergency.
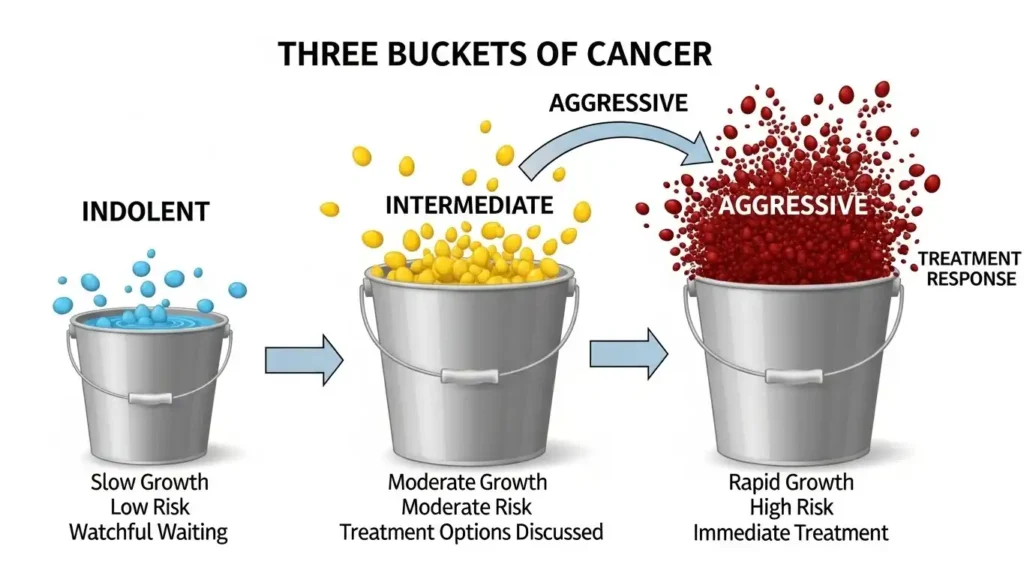
The Concept of Overdiagnosis Overdiagnosis is finding a condition that would never have hurt you if it stayed hidden. We think of cancer in three buckets:
- Indolent: These grow so slowly they will never cause symptoms.
- Intermediate: These grow slowly but steadily. This is the “sweet spot” for screening.
- Aggressive: These move so fast that a random yearly scan might miss them anyway.
Pro Tip: Focusing on “indolent” findings often leads to “treatment” for a disease that was never going to make you sick. 💡
Real-World Consequences: When “Just Checking” Goes Wrong
The “Cascade of Care” Once a scan finds a tiny spot, the “cascade of care” begins. One unclear finding leads to more scans, which lead to biopsies, which can lead to surgery.
Case Study: The Thyroid Cancer Epidemic In South Korea, screening for thyroid nodules became very common. Diagnoses went up by 11 times. Thousands of people had their thyroids removed. However, the number of people dying from thyroid cancer did not change at all. The harm was real: many suffered nerve damage or became dependent on hormones for life, all for a cancer that wasn’t going to kill them.
Case Study: The Lung Nodule Nightmare I remember a story of a patient who got a shoulder MRI. The edge of the scan caught a tiny lung nodule. This led to a chest CT, then a PET scan, and then a pelvic MRI. Eventually, she had a hysterectomy for benign fibroids. She suffered a major infection and lived in terror for a year. All of this started from a benign spot on her lung that had nothing to do with her shoulder pain.
Psychological Harms (“Scanxiety”) Waiting for results creates “scanxiety.” Studies show 10% to 30% of patients feel significant anxiety while waiting. You go from being a healthy “walkie-talkie” person to a “patient” overnight. Is the “peace of mind” worth months of fear?
Better Ways to Spend $2,500 on Your Health
The Opportunity Cost of MRI If you have $2,500, spending it on a scan might be the least effective way to stay healthy. Instead, you could hire a personal trainer and a dietitian for a year.
The Power of Prevention Over 50% of diseases are tied to things we can change. In fact, 70% to 80% of heart disease is preventable.
High-Value Action Items:
- Aerobic and strength training.
- Stopping smoking (the biggest win for your health).
- Checking your cholesterol, blood sugar, and blood pressure.
Dr. Davenport notes that if these scans saved lives, insurance companies would pay for them. It is cheaper to treat a small problem than a big one, yet insurance companies still say “no” to random full-body MRIs.
Navigating Specific Screenings: What Actually Works?
Prostate MRI screening benefits: A Game Changer
Unlike full-body scans, a targeted prostate MRI screening benefits men by finding the right problems. This technology has changed how we work. It helps us find clinically significant prostate cancer while letting us ignore the “indolent” ones.
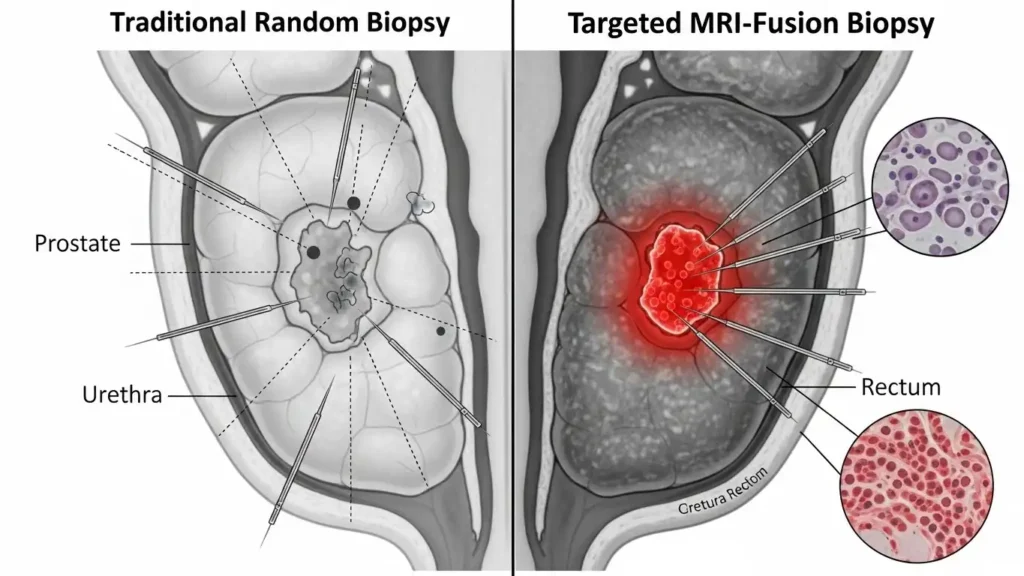
The Stat and the Caveat A high-quality Multiparametric MRI has a 95% negative predictive value. This means if the scan is clear, you are almost certainly safe. However, the false-positive rate can be 40-60%. This is why you need a specialist to look at the Gleason score interpretation and decide if you really need a targeted vs random biopsy.
Coronary Calcium Scores (Heart CT) This is a great test for certain people to see their heart risk. But it also uses radiation and can find those pesky “incidentalomas” in your lungs. Always use a risk calculator before getting one.
The Future of Medical Imaging: AI and Innovation
Will AI Replace Radiologists? AI is not taking over yet. It will likely take 10 to 20 years before AI could even think about replacing a human doctor. Currently, AI helps make scans faster and helps ensure the PSA screening accuracy is backed by better data.
Ky-RADS and Future Precision New systems like Ky-RADS for kidneys are being built. These help us decide if a tumor is “aggressive” or “lazy.” This helps men choose “active surveillance” (watching the spot) instead of rushing into surgery.
Enhancing Prostate MRI screening benefits with AI
AI is currently used to reconstruct images faster. This makes the MRI experience shorter and more comfortable for you.
A Patient’s Guide to Safe Imaging
Questions to Ask Your Provider If you need an MRI with contrast, ask if they use a “macrocyclic” agent. These are very stable and safe. If you are looking into prostate cancer detection, ask if the radiologist specializes in prostates.
Pro Tip: Always ask your facility if they track their “biopsy correlation” to see how accurate their scans actually are. 🎯
Understanding Contrast Dye
- Gadolinium (MRI): Very safe. Serious reactions happen in only about 1 in a million people.
- Iodine (CT): Can make you feel a “warm flush.” This is normal, not an allergy.
Getting Your Results Because of the “Cures Act,” you might see your report on your phone before I do. If you see the words “carcinoma not excluded,” do not panic. This is “doctor-speak” that often just means the scan wasn’t 100% perfect. Waiting a few days to talk to your doctor is much better for your mental health.
Conclusion: Defining “High Value” Care
The Bottom Line Value in health is your outcome divided by the cost. A test is only valuable if it changes what we do and helps you live longer or better.
How effective is prostate MRI at distinguishing between aggressive cancer and indolent disease that doesn’t require treatment? It is very effective when used correctly by a specialist, but it is not a magic wand.
Final Call to Action Don’t get distracted by expensive trends. Stick to the basics:
- Follow evidence-based rules for colonoscopies and lung screenings.
- Focus on diet, exercise, and sleep.
- Talk to a urologist who cares about your quality of life.
Your health is a journey, not a single scan. Let’s focus on the things that truly help you thrive.